.png)
What is prior authorization appeal AI and how does it work
Prior authorization appeal AI is software that helps healthcare practices challenge insurance denials and overturn rejected claims. When a payer denies a prior authorization request, these AI tools analyze the denial reason and identify missing documentation. They then generate appeal letters that address the specific criteria the insurer requires.
Prior authorization itself is the process where insurers require advance approval before covering a medication, procedure, or service. When that approval is denied, practices have the right to appeal.
Traditionally, appeals require staff to manually review denial letters and gather supporting clinical documentation. Staff must then write persuasive letters citing medical necessity and submit everything through payer portals or fax.
AI changes this by automating the most time-consuming steps. The software reads the denial reason, pulls relevant clinical data, and matches documentation against payer-specific criteria.
It then drafts an appeal letter that directly addresses why the denial was inappropriate. What used to take nearly an hour can now take under five minutes.
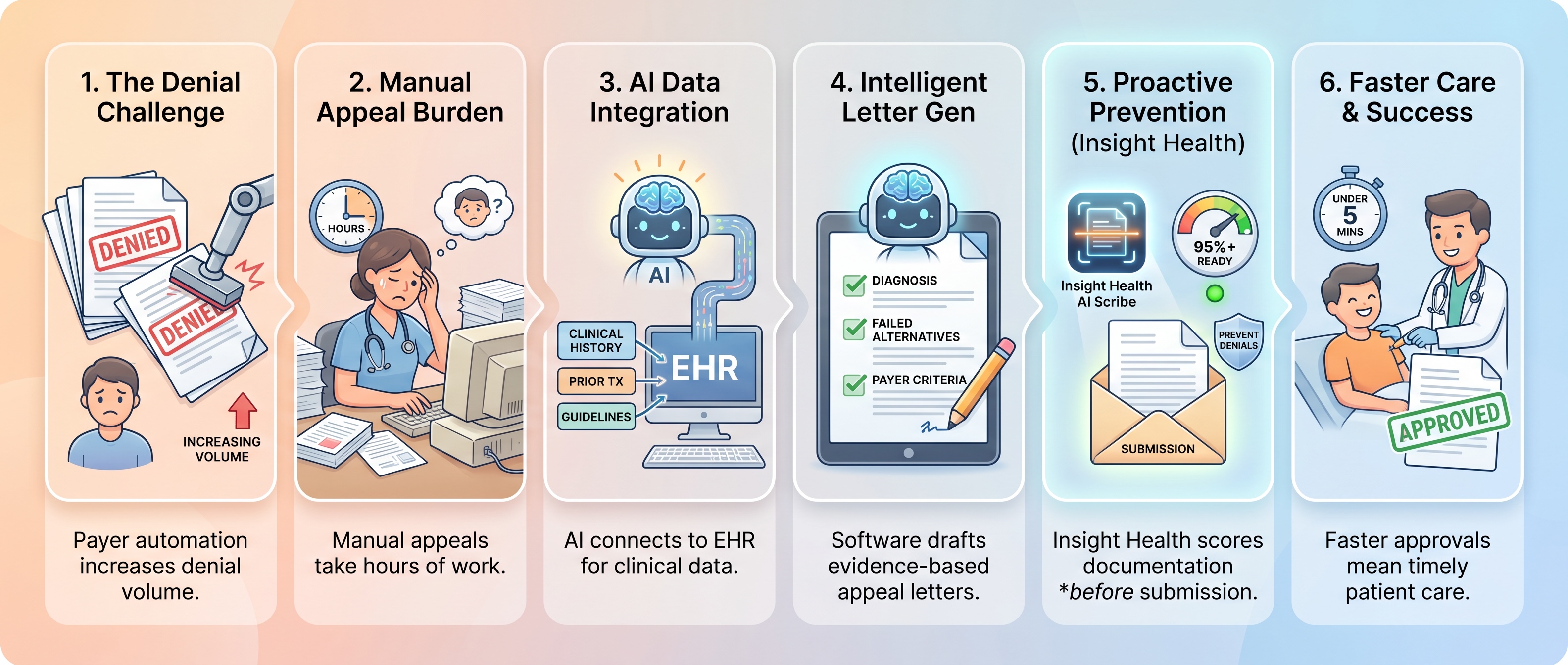
Why prior authorization denials are increasing
Insurance companies are using their own AI and automated decision-making systems to process prior authorization requests at scale. Learn more about how Medicare's WISeR model is expanding AI-driven authorization to traditional Medicare. These automated systems can issue batch denials with minimal human review, creating more barriers between patients and necessary care.
The volume of prior authorizations has also grown significantly. Physicians report that prior authorization requirements have increased over the last five years, and practices are struggling to keep up with the appeal workload. More requests mean more opportunities for denials.
Denials have real consequences for your patients. When appeals don't happen or happen too slowly, patients delay treatment or abandon it entirely, with 82% of physicians reporting prior authorization can lead to treatment abandonment.
Some patients end up in the emergency department because they couldn't get timely approval for the care they needed.
How AI automates the appeal process
AI appeal tools work by connecting to your EHR and pulling the clinical documentation that supports medical necessity. When a denial comes in, the AI identifies what information the payer claims is missing or insufficient, then locates that evidence in the patient's chart.
The software generates a complete appeal letter that includes:
The best AI appeal systems are trained on payer-specific requirements. They know what eviCore, Cigna, UnitedHealthcare, and other major payers look for in their medical necessity determinations. This specificity matters because a generic appeal letter is far less likely to succeed than one that speaks directly to the criteria that payer uses.
Real-time documentation prevents denials before they happen
The most effective approach to prior authorization appeals is preventing denials in the first place. AI systems that capture clinical encounter data in real time can score documentation against payer criteria before submission.
If the documentation is complete, the request goes out automatically. If something is missing, the system flags it immediately so you can fix it before the denial ever occurs.
At Insight Health, our Prior Authorization Automation works this way. Because our AI Scribe captures clinical details during the encounter, we can evaluate documentation completeness before the visit even ends. The system detects ICD-10 coding errors, identifies missing clinical elements, and routes cases through intelligent branches based on readiness scores.
When documentation scores above 95% readiness, the PA request submits automatically with zero manual data entry. When minor gaps exist, the system prompts coordinators to fill them. When critical clinical details need clarification, providers receive micro-questionnaires that take seconds to complete.
This approach targets first-pass approval rates well above the industry average. For pain management practices performing epidural steroid injections, our PA automation reduces submission time from 45 minutes to under five minutes.
What makes a prior authorization appeal successful
Successful appeals share common characteristics. They directly address the specific denial reason with concrete clinical evidence. They don't simply restate the original request or provide generic justifications.
The appeal must give the medical reviewer a reason to overturn the initial denial with documentation they can defend to their organization.
Strong appeals include these elements:
Prior authorization appeal AI tools excel at assembling these elements quickly and consistently. Our Prior Authorization Automation is built to handle exactly this kind of structured, evidence-based appeal generation.
They don't forget to include relevant history or miss a citation that could strengthen the case. And because they're trained on what works, they structure arguments in ways that medical reviewers find persuasive.
The cost of manual appeals
The administrative burden of prior authorization appeals is substantial. On average, physicians and their staff spend 13 hours per week completing prior authorization work for a single physician. 40% of physicians have staff whose sole job is handling these requests.
When your staff is overwhelmed, some denials go unchallenged. Many physicians report doubts about whether appeals will succeed based on past experience, and others say they lack sufficient resources to file appeals at all.
With 80.7% of appealed denials overturned in Medicare Advantage, every unchallenged denial represents lost revenue and a patient who may not receive needed care. When you add up the staff hours, the missed approvals, and the patients who give up, the true cost of manual appeals becomes clear.
Preparing for CMS-0057-F compliance
The Centers for Medicare and Medicaid Services finalized rules requiring payers to implement electronic prior authorization by January 2027. This regulation, known as CMS-0057-F, mandates that payers support FHIR-based Prior Authorization Support APIs. FHIR is a standard for exchanging healthcare information electronically, and these APIs will enable real-time electronic submission and status checking.
Practices that adopt prior authorization appeal AI tools now will be positioned for this transition. Systems built with FHIR PAS API readiness can connect directly to payer systems once the mandate takes effect, further reducing manual work and accelerating approvals.
The regulatory environment is also shifting toward greater transparency, with initiatives like Medicare's WISeR model introducing AI-assisted prior authorization review for traditional Medicare. Payers will be required to provide specific reasons for denials and respond within defined timeframes.
AI tools that track these requirements and flag violations give practices leverage in the appeal process. If a payer misses a deadline or fails to provide adequate justification, you'll know immediately.
How to evaluate AI prior authorization appeal tools
When selecting a prior authorization appeal AI solution, consider factors that determine whether the tool reduces your workload. You want a solution that helps, not just another system to manage.
Practices performing high-volume procedures like epidural steroid injections, imaging studies, or specialty medications see the greatest return from AI prior authorization tools. The time savings compound quickly when you're processing dozens of requests per week.
At Insight Health, we built our Prior Authorization Automation with practicing physicians who understand these workflows firsthand. Our co-founders include a neurosurgeon and a cardiologist who have experienced the frustration of prior authorization denials in their own practices. That clinical perspective shapes every feature we build.
FAQ
How long does a prior authorization appeal take to get a decision?
Standard appeals typically take 30 days for a decision from the payer. Expedited appeals for urgent situations must be reviewed within 72 hours. AI tools can prepare and submit appeals within minutes, but payer response times remain governed by regulations and internal processes.
What should I do if my first prior authorization appeal is denied?
Most insurance plans allow multiple levels of internal appeal, typically two or three. If internal appeals fail, you can request external review through an independent reviewer or state process. External reviews statistically favor patients, so persistence matters when treatment is medically necessary.
Who can write prior authorization appeals?
Billing staff can draft appeal letters and gather documentation, but the physician must sign because appeals require clinical judgment about medical necessity. Our AI Scribe captures the clinical detail needed to support these appeals during the encounter itself. AI tools help by generating the clinical content that physicians can review and approve quickly, reducing the time burden on providers while maintaining appropriate oversight.

Get Started
AI-Enhanced Healthcare with Insight Health


