
How AI prior authorization software works
AI prior authorization software is a platform that automates the approval process providers must complete before delivering certain treatments or medications. Instead of staff manually gathering documents, filling out prior auth forms, and waiting on hold with payers, the software handles these steps automatically.
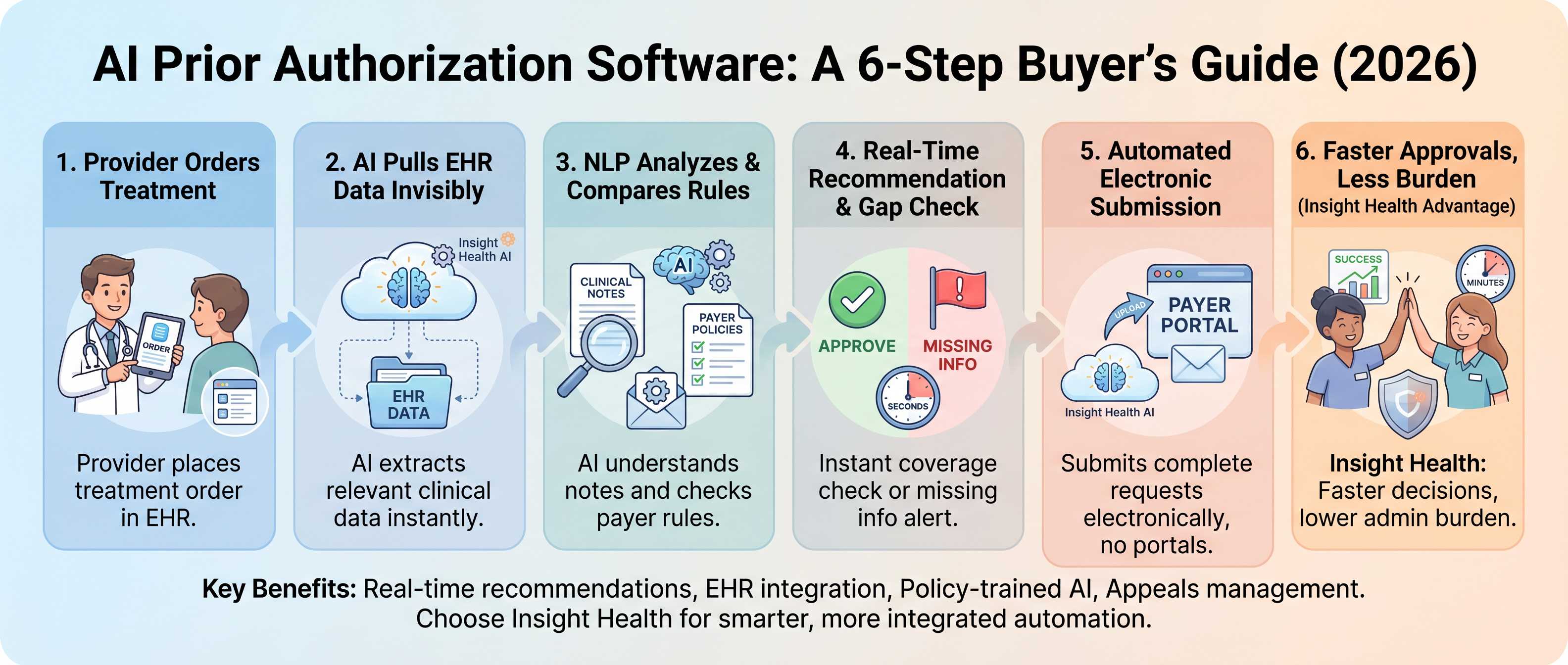
The process starts when a provider orders a treatment that requires authorization. The software pulls the relevant clinical data directly from your electronic health record. Then it compares that documentation against the specific payer's medical necessity criteria using natural language processing, which is AI that can read and understand clinical notes the way a human would.
If the documentation meets the payer's requirements, the system submits the request electronically. If something is missing, it flags exactly what you need to add before submission. This means you find out about documentation gaps before they cause a denial, not after.
The best platforms work invisibly within your existing EHR. Your staff doesn't need to log into a separate portal or learn a new system. They order the treatment, and the AI handles the rest in the background.
Key features to evaluate
Not all AI prior authorization platforms work the same way. When you're comparing options, focus on the capabilities that will actually reduce your team's workload and improve your approval rates, according to Medical Economics, early adopters report first-pass approval rates above 95%.
Real-time recommendations
- What it does: Analyzes clinical data and tells you within seconds whether documentation is complete.
- Why it matters: You know immediately if a treatment will be covered instead of waiting days.
EHR integration
- What it does: Pulls patient data from your existing system and submits requests electronically.
- Why it matters: Your staff doesn't need to re-enter information or switch between systems.
Specialty support
- What it does: Handles specific benefit types like pharmacy, radiology, or psychiatric authorizations.
- Why it matters: You don't need separate tools for different types of treatments.
Policy-trained AI
- What it does: Maintains current rules for hundreds of payers and updates automatically.
- Why it matters: You stay compliant with changing requirements without manual tracking.
Appeals management
- What it does: Generates resubmissions and denial defense letters when authorizations are rejected.
- Why it matters: You spend less time on back-and-forth when payers initially say no.
Top AI prior authorization vendors
The market includes platforms built for health plans, providers, and pharmacies. Each vendor approaches automation, integration, and pricing differently. Here's what you need to know about the major players.
Availity AuthAI
Availity AuthAI is a payer-focused platform that delivers authorization recommendations in under 90 seconds. The system uses analytical AI with transparent logic, meaning you can see exactly how it reached each recommendation. This matters because some AI systems are "black boxes" that don't explain their reasoning.
The platform is built for CMS-0057 compliance, which is the federal rule requiring payers to support electronic prior authorization by January 2027. If you're a health plan preparing for that deadline, Availity is already ready.
- Best for: Health plans that want auditable AI decisions and regulatory compliance.
- Limitation: Providers access it through their health plans, not directly.
- Pricing: Enterprise SaaS model, contact for quote.
Myndshft
Myndshft handles both medical and pharmacy prior authorizations in one platform. The system maintains rules for over 600 payers and uses a self-learning engine that adapts when payer policies change. This means your team doesn't need to manually track policy updates.
The platform reduces manual workflow time from roughly 50 minutes per authorization to under 5 minutes. DrFirst acquired Myndshft in 2024, which gives it access to a network of 270 EHRs.
- Best for: Organizations that need unified medical and pharmacy authorization in one system.
- Limitation: The acquisition may affect the product roadmap.
- Pricing: Enterprise SaaS model, contact for quote.
Cohere Health
Cohere Health serves health plans with a complete utilization management suite. The platform includes AI copilot tools that help clinical reviewers find relevant evidence faster when manual review is needed. It also connects prior authorization decisions to claims validation, which helps catch payment issues before they become problems.
The system offers personalized authorization programs rather than one-size-fits-all rules. This means different provider groups can have different workflows based on their performance and specialty.
- Best for: Health plans that want to connect authorization decisions to payment integrity.
- Limitation: Designed for payers, not providers.
- Pricing: Per-member-per-month for health plans, contact for quote.
CoverMyMeds
CoverMyMeds is free for providers and pharmacies, which makes it the most accessible option for practices with limited budgets. The platform connects to over 900,000 providers and 50,000 pharmacies, giving it the broadest network in the market.
The system was originally built for pharmacy prior authorizations. Recent acquisitions are expanding its medical authorization capabilities, but pharmacy remains its strength.
- Best for: Providers and pharmacies that want free electronic prior authorization with broad payer connectivity.
- Limitation: Medical prior authorization features are newer and less mature.
- Pricing: Free for providers and pharmacies. Enterprise programs require sales engagement.
EthermedAI
EthermedAI automates the complete prior authorization workflow without requiring you to use a separate portal. The AI is pre-trained on over 100,000 payer policies, so it knows what each payer requires before you submit.
The platform handles all authorization types: prospective (before treatment), concurrent (during treatment), and retrospective (after treatment). It also generates denial defense letters automatically when authorizations are rejected.
- Best for: Organizations that want invisible automation within their existing EHR.
- Limitation: Smaller company with less market presence than established vendors.
- Pricing: Enterprise SaaS model, contact for quote.
Availity AuthAI vs. Myndshft
These two platforms take different approaches to solving the same problem. Understanding the differences will help you choose the right fit.
Real-time decision-making
Availity delivers recommendations in under 90 seconds using transparent AI that shows its reasoning. Myndshft focuses on reducing total workflow time from 50 minutes to under 5 minutes. Availity emphasizes speed of the initial recommendation. Myndshft emphasizes eliminating manual work throughout the entire process.
Payer and benefit coverage
Availity is a payer-side solution that providers access through their health plans. Myndshft works directly with providers and handles both medical and pharmacy benefits in one platform with rules for over 600 payers. If you need both benefit types in one system, Myndshft offers broader coverage.
Integration approach
Both platforms integrate via APIs with existing systems. Availity uses FHIR APIs, which is the standard for healthcare data exchange. Myndshft embeds in EHRs, revenue cycle systems, and health information exchanges. Myndshft's access to the DrFirst network may give it an edge for EHR connectivity.
CoverMyMeds vs. EthermedAI
These platforms differ most in their business model and authorization scope.
Network and adoption
CoverMyMeds has the largest network with connections to over 900,000 providers and 50,000 pharmacies. EthermedAI focuses on seamless EHR integration without separate portals. If broad network reach matters most, CoverMyMeds wins. If workflow simplicity matters most, EthermedAI wins.
Authorization scope
CoverMyMeds started with pharmacy authorizations and is expanding into medical. EthermedAI handles medical, pharmacy, and all authorization types from the start. For comprehensive medical prior authorization, EthermedAI offers more mature capabilities today.
Cost to providers
CoverMyMeds is free for providers and pharmacies. EthermedAI uses enterprise pricing with custom quotes. If budget is your primary constraint, CoverMyMeds eliminates upfront costs entirely.
Which AI prior authorization software should you choose
Your choice depends on three factors: whether you're a provider or payer, what types of benefits you manage, and how much integration complexity you can handle.
- Choose Availity AuthAI if: You're a health plan that needs transparent, auditable AI decisions and CMS-0057 compliance.
- Choose Myndshft if: You need medical and pharmacy authorization in one platform with automatic policy updates.
- Choose Cohere Health if: You're a health plan connecting authorization decisions to claims validation and payment integrity.
- Choose CoverMyMeds if: You're a provider prioritizing free access and broad network connectivity, especially for pharmacy authorizations.
- Choose EthermedAI if: You want automation that works invisibly within your existing EHR without adding another portal.
Getting started with AI prior authorization software
Implementation starts with a demo to assess your current clinical workflow, integration requirements, and authorization volume. Most vendors need either direct EHR integration or connection through existing health information networks.
Before committing to any platform, verify that your EHR appears on the vendor's integration list. If you're a health plan, confirm that the platform works with your existing utilization management and claims systems. Ask about implementation timelines, training requirements, and ongoing support.
The fastest implementations happen when organizations already have integrated EHR systems and clear documentation standards. If your current processes are fragmented or heavily manual, you may need workflow redesign, starting with clinical documentation, before the platform delivers full value.
FAQ
What is the difference between prior authorization and utilization management?
Prior authorization is one specific type of utilization management where providers must get payer approval before delivering certain treatments. Utilization management is the broader category that also includes concurrent review during treatment and retrospective review after treatment.
How long does AI prior authorization typically take?
Leading platforms deliver authorization recommendations in under two minutes by analyzing clinical information against payer policies. The total time to final determination depends on whether the payer requires additional information or manual clinical review.
Can AI prior authorization software handle all benefit types?
Most platforms handle medical and pharmacy prior authorizations, though some specialize in one category. Check vendor documentation to confirm coverage for your specific benefit types and payer network before purchasing.
Do I need to change my EHR to use AI prior authorization software?
No. Most platforms integrate with existing EHRs through APIs or direct connections. Verify that your specific EHR appears on the vendor's supported integration list before making a decision.
What happens if the AI makes a wrong recommendation?
Platforms like Availity AuthAI use recommendation engines that don't auto-approve or auto-deny, so payers retain final control. Other platforms flag high-risk cases for manual review. All recommendations should be auditable so you can see the reasoning behind each decision.

Get Started
AI-Enhanced Healthcare with Insight Health


