.png)
What is prior authorization in pain management
Prior authorization is a requirement from insurance companies that you must get approval before delivering certain treatments, medications, or procedures. In pain management, this means you cannot prescribe specific medications or perform interventional procedures until the insurer confirms they will cover the service. The process exists because insurers want to verify that treatments are medically necessary and align with their coverage guidelines.
Insurance companies require prior authorization pain management approvals for several reasons. They want to control costs by ensuring patients receive evidence-based care rather than unnecessary procedures. They also want to reduce risks associated with certain medications, particularly opioids, which carry addiction and overdose concerns.
For insurers, prior authorization serves as a checkpoint to confirm that conservative treatments have been attempted before approving more expensive interventions.
Many pain management treatments require prior authorization before you can proceed. Opioid prescriptions almost always need approval, especially for long-term use or higher doses. Epidural steroid injections for back and neck pain typically need insurer approval before scheduling.
Radiofrequency ablation, which blocks nerve signals to reduce chronic pain, requires authorization in most cases. Spinal cord stimulators need extensive documentation and approval for both the trial and permanent implantation. Newer specialty medications and biologics often have the strictest prior authorization requirements of all.
Prior authorization is different from a referral. A specialist referral is when a primary care provider directs a patient to another provider for evaluation or treatment. Prior authorization is when you ask the insurer to approve a specific treatment or medication.
Some patients need both, depending on their insurance plan.
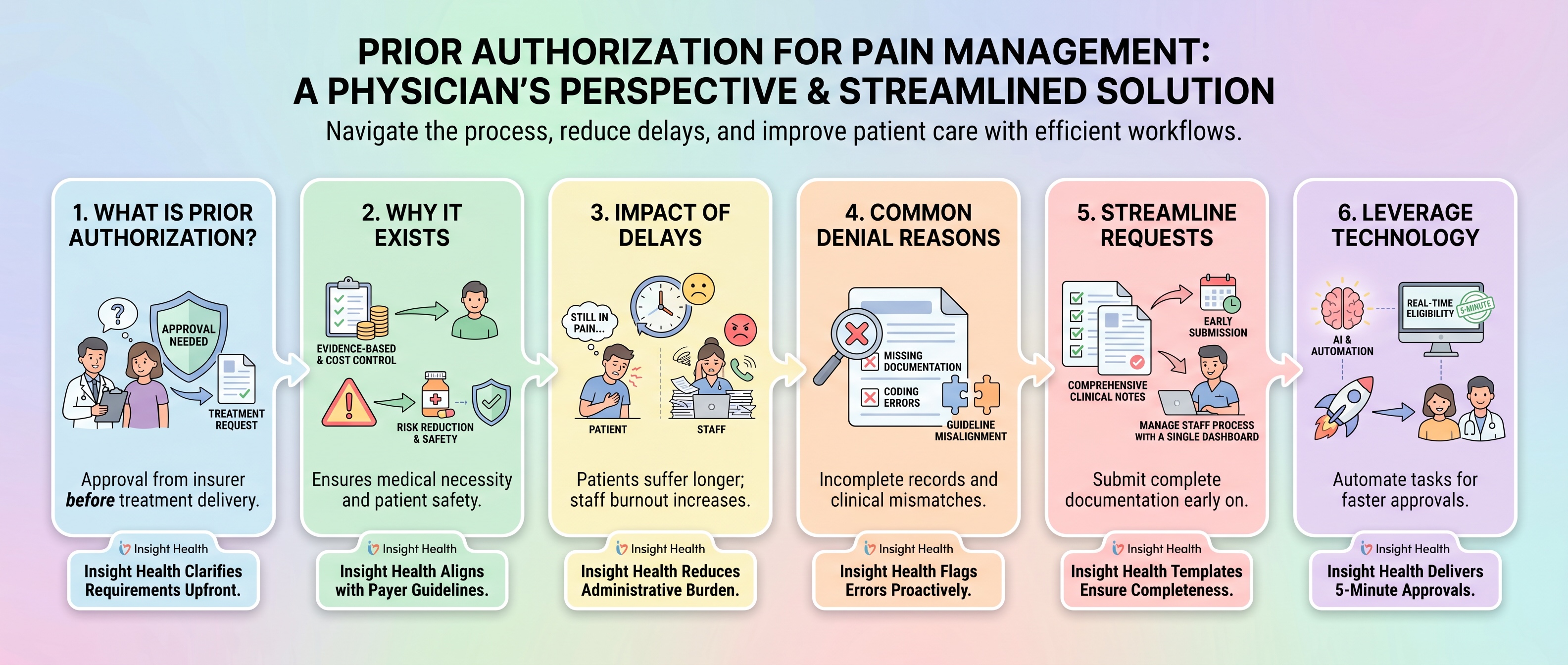
The impact of prior authorization pain management delays on patient care
When prior authorization takes days or weeks, patients remain in pain longer than necessary. I have seen patients wait two to three weeks for approval on procedures that could provide immediate relief.
During this time, their condition may worsen and their quality of life suffers. They may also turn to emergency rooms for care that could have been prevented.
The administrative burden falls heavily on clinical staff. My team spends an average of 45 minutes per prior authorization request. This includes gathering documentation, submitting forms, calling insurers, and following up on pending requests.
An AMA survey found physicians and staff spend 13 hours per week on prior authorizations, time that could be spent on direct patient care. Our guide on the true value of AI in clinical practice explores how reducing this burden improves physician retention.
Staff burnout is a real consequence when employees spend their days fighting with insurance companies instead of helping patients. Our guide on the true value of AI in clinical practice explores how reducing administrative burden improves physician retention.
The repetitive nature of prior authorization work, combined with frequent denials and delays, creates frustration that leads to turnover. Replacing trained staff costs time and money that most practices cannot afford.
Patient retention also suffers when prior authorization creates friction. Patients who experience repeated delays may lose trust in their provider or seek care elsewhere.
An AMA survey found that 82% of physicians say prior authorization can lead patients to abandon their treatment plans entirely. This is particularly concerning in pain management, where untreated pain can lead to depression, disability, and decreased function.
Common reasons prior authorization pain management requests are denied or delayed
Understanding why insurers deny prior authorization pain management requests helps you prevent those denials in the first place. Most rejections come down to documentation issues or misalignment with insurer guidelines.
Incomplete or missing documentation is the most common reason for denial. Insurers need specific clinical justification, including patient history, physical exam findings, imaging results, and previous treatment records. If any piece is missing, the request gets delayed or denied.
You may know the treatment is appropriate, but the insurer only sees what you submit.
Treatment not aligned with insurer guidelines causes many denials. Each insurance company has its own criteria for what qualifies as medically necessary. A treatment you consider appropriate may not meet their specific evidence-based protocols.
These guidelines vary by payer and change frequently, making it difficult to keep up.
Lack of prior treatment attempts triggers denials for interventional procedures. Many insurers require step therapy, meaning patients must try and fail conservative treatments like physical therapy or oral medications before approving more expensive interventions. If you cannot document that the patient tried these approaches, the insurer will reject the request.
Coding or clinical indication mismatches cause preventable denials. If the diagnosis code does not align with the requested treatment, insurers will reject the request. A simple coding error can delay care by weeks.
The ICD-10 code must match the procedure code and support the medical necessity of the treatment.
How to streamline prior authorization pain management requests
Preparation is the most effective way to reduce prior authorization pain management delays. Submitting complete, accurate requests the first time prevents the back-and-forth that extends approval timelines.
Prepare comprehensive clinical documentation upfront
Before submitting any request, ensure the documentation includes everything the insurer needs to make a decision. This means the patient's complete history, all failed treatments with dates and outcomes, and current pain scores.
Also include functional limitations and a clear clinical rationale for the requested procedure. Insurers want to see that you have considered alternatives and that this treatment is the appropriate next step.
Include imaging results that support your clinical findings. For procedures like epidural steroid injections or radiofrequency ablation, insurers expect to see MRI or CT findings that correlate with the patient's symptoms. Highlight the specific findings in the radiologist's report that justify the procedure.
Know your insurer's specific requirements
Each insurance company has different submission rules, required forms, and clinical criteria. What works for one payer may not work for another. I keep a reference guide for our most common payers so staff know exactly what each insurer expects.
Some insurers use third-party vendors like eviCore to manage prior authorization for certain procedures. Our overview of Medicare's WISeR prior authorization model explains how new payer programs are changing submission requirements.
These vendors have their own portals, forms, and clinical criteria. Knowing which vendor handles which services for each payer prevents wasted time submitting to the wrong place.
Submit requests early in the treatment planning process
Initiate prior authorization as soon as you determine a patient needs a specific treatment, not when they are ready to schedule. This gives the insurer time to process the request without delaying the patient's care. If you wait until the patient is on the schedule, any delay in approval becomes a delay in treatment.
Designate a single point of contact
One staff member should track each request from submission to approval. This prevents miscommunication and ensures nothing falls through the cracks. That person knows the status of every pending authorization and can follow up proactively.
Follow up proactively
If you have not received a response within three business days, call the insurer directly. Waiting passively for a response often extends timelines unnecessarily. A quick phone call can move a request from pending to approved.
Leveraging technology to reduce prior authorization burden
Technology can eliminate much of the manual work that makes prior authorization pain management so time-consuming. The right tools help your team submit accurate requests faster and track approvals without constant phone calls.
Automated documentation templates ensure consistent, complete submissions every time. Instead of starting from scratch, staff use templates that prompt them to include all required information. This reduces errors and speeds up the submission process.
Real-time eligibility checks verify coverage and requirements before you submit a request. You can see whether a treatment requires prior authorization, which vendor handles the request, and what documentation the insurer expects. This prevents wasted effort on requests that were never going to be approved.
Integrated tracking systems monitor request status across all payers in one place. Instead of logging into multiple portals or making phone calls to check status, staff can see everything in a single dashboard. This saves time and ensures no request gets lost.
AI-assisted prior authorization platforms can flag missing information and suggest insurer-specific language before submission. Some systems score documentation completeness and predict approval likelihood, allowing your team to address gaps before they cause denials.
Platforms built by physicians understand clinical workflows better than generic administrative tools. They know what documentation pain management procedures require and can prompt staff to include the right information. See how our AI front desk tools reduce administrative load across your practice.
For pain management practices performing epidural steroid injections, AI-powered prior authorization can reduce submission time from 45 minutes to under 5 minutes. These systems capture clinical encounter data in real time and score documentation against payer-specific criteria. They also detect coding errors before they cause denials and submit requests through payer portals with zero manual data entry.
Best practices for prior authorization pain management
Reducing prior authorization pain management friction requires a systematic approach, not just individual effort. I have implemented several workflow changes that have measurably improved our approval rates and reduced turnaround times. Our guide to reducing clinic staff burnout covers related workflow strategies.
The goal is to make prior authorization a predictable, manageable part of your workflow rather than a constant source of frustration. With the right systems and processes in place, you can reduce denials, speed up approvals, and get patients the care they need faster.
Frequently asked questions about prior authorization pain management
How long does prior authorization for pain management procedures typically take?
Timelines vary by insurer, but most decisions are made within three to five business days if documentation is complete. As of 2026, CMS requires responses within 72 hours for urgent requests and seven calendar days for standard requests.
Can I appeal a prior authorization denial for a pain management treatment?
Yes, most insurers have an appeal process that allows you to submit additional clinical evidence or request peer-to-peer review with their medical director. Many denials are overturned on appeal when you provide the right documentation.
Care options while awaiting prior authorization
You can often request expedited review or emergency authorization based on clinical need. Document the urgency and submit directly to the insurer's medical review team.
Are all pain management treatments subject to prior authorization?
No, coverage varies by insurer and plan. Some treatments are pre-approved, while others require authorization.
Verify each patient's specific plan requirements before assuming authorization is needed. Our AI Virtual Care Assistant can help verify coverage requirements before each visit.
How can I reduce prior authorization denials for pain management procedures?
Submit complete clinical documentation upfront and ensure your diagnosis codes match the requested treatment. Document failed prior treatments and align your request with the insurer's evidence-based guidelines.

Get Started
AI-Enhanced Healthcare with Insight Health


