
What is the CMS-0057-F prior authorization rule?
CMS-0057-F is a federal regulation that requires health insurers to use standardized digital systems for processing prior authorization requests. Prior authorization is when your practice needs approval from a payer before providing certain treatments or services. This rule replaces manual phone calls and faxes with automated electronic submissions.
The Centers for Medicare and Medicaid Services issued this rule because the current prior authorization process wastes enormous amounts of time. Practices submit requests by phone or fax, wait days for responses, and often resubmit because of missing information. CMS-0057-F creates a standardized digital framework that all covered payers must follow.
The rule requires payers to build application programming interfaces, commonly called APIs. An API is a digital connection that lets two computer systems talk to each other automatically. With these APIs in place, your EHR can send prior authorization requests directly to payers and receive decisions without anyone picking up a phone.
This rule applies to Medicare Advantage plans, Medicaid managed care organizations, CHIP programs, and qualified health plan issuers on federal and state health insurance exchanges. Traditional Medicare fee-for-service, employer group health plans, and self-insured plans are not required to comply.
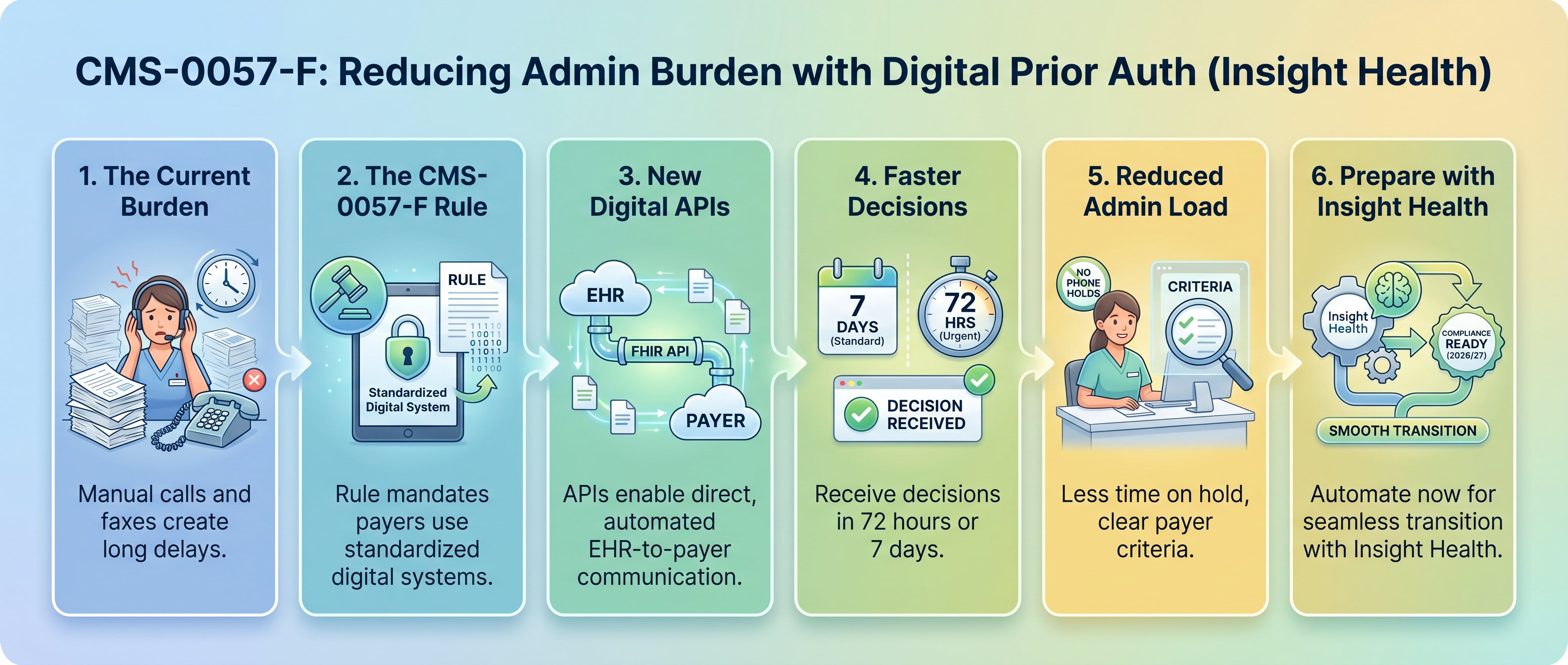
Why prior authorization reform was needed
Prior authorization exists to control healthcare costs by requiring payer approval before certain treatments. The problem is that the current process creates massive delays and administrative burden. Your staff spends hours on hold, faxing documents, and following up on requests that should take minutes.
The pain points are familiar to anyone who has worked in a medical practice:
These problems compound each other. A denial means resubmission, which means more waiting, which means more delayed care. CMS recognized that this cycle harms patients and burns out clinical staff. The rule aims to break that cycle through standardized, real-time digital communication.
Key requirements of the CMS-0057-F rule
The rule establishes several new APIs that payers must build and maintain. Each API serves a specific purpose in streamlining how practices and payers exchange information.
Prior Authorization API
The Prior Authorization API is the core of this rule. Payers must build a FHIR-compliant system that accepts prior authorization requests in a standardized digital format. FHIR stands for Fast Healthcare Interoperability Resources. It is a technical standard that ensures all healthcare systems can communicate using the same language.
Instead of calling or faxing requests, your practice management system or EHR submits prior authorization requests electronically. The payer's system receives the request, processes it, and sends back a decision. This happens in real time or near-real time for most request types.
Provider Access API
The Provider Access API gives your practice direct access to request status and payer requirements. You can check where a pending request stands without calling the payer. You can also see exactly what documentation the payer needs before you submit or resubmit.
This eliminates the frustrating loop of calling for updates and being told the request is still under review. Your staff gets answers immediately through the API instead of waiting on hold.
Patient Access API
The Patient Access API lets patients see their own prior authorization information through a portal or app. They can check request status and read decision reasons without calling your office.
This matters for your practice because it reduces incoming phone calls. When patients can self-serve for status updates, your front desk handles fewer inquiries about authorization timing.
Payer-to-payer data exchange
When a patient switches insurance plans, the new payer can request prior authorization history from the previous payer electronically. This prevents patients from having to restart the authorization process from scratch every time their coverage changes.
For your practice, this means fewer resubmissions when patients change plans mid-treatment. Continuity of care is maintained without extra administrative work on your end.
How CMS-0057-F impacts medical practices
The rule creates measurable changes in how your practice handles prior authorization. These changes affect decision speed, staff workload, and your visibility into payer requirements.
Faster prior authorization decisions
Most requests will receive decisions within hours instead of days. The rule establishes specific timeframes that payers must meet. Urgent requests must receive responses within 72 hours. Standard requests must receive responses within seven calendar days.
Your staff no longer waits in phone queues hoping for updates. Decisions arrive electronically and route automatically to the right person. Patients can start treatment sooner because you are not waiting on payer responses.
Reduced administrative burden
Fewer phone calls, faxes, and manual data entry means your staff spends less time on prior authorization tasks. Requests flow directly from your EHR to payers through the standardized APIs.
Currently, 92% of practices dedicate staff solely to managing prior authorization volume. That time can shift to patient care or other activities.
The time your billing and clinical staff currently spend on prior authorization can shift to patient care or other activities. This also helps with staff satisfaction and retention. Nobody enjoys spending their day on hold with insurance companies.
Greater transparency into payer criteria
Payers must clearly document their authorization criteria and explain their decision reasoning. Your practice gains insight into why requests are approved or denied before you submit.
You can adjust your workflows to align with payer requirements proactively. When you understand criteria upfront, you reduce denials. Fewer denials means fewer appeals and a faster revenue cycle.
Which payers must comply with CMS-0057-F?
Not all payers fall under this rule. Understanding which ones do helps you plan your preparation.
If your patients receive coverage from any of the covered payer types, those payers must meet CMS-0057-F requirements by the compliance deadlines. Your practice benefits regardless of which specific payers your patients use within those categories.
CMS-0057-F compliance timeline
The rule establishes two major compliance deadlines. Both payers and practices need to prepare for these dates.
January 2026 deadlines
Payers must have functioning APIs available for testing and integration by January 2026. Your EHR and practice management system vendors will begin integration work during this period. You may be asked to test connectivity with specific payers.
Start conversations with your technology vendors now about their CMS-0057-F roadmap. Ask for specific dates, not vague commitments. You need to know when your systems will be ready.
January 2027 deadlines
All APIs must be fully operational by January 2027. Payers must accept and respond to electronic prior authorization requests through the standardized system. Patient Access APIs must also be available.
This is when your practice transitions from manual to digital prior authorization workflows. Make sure your EHR and billing systems are updated and integrated before this date. Train your staff on the new workflows so the transition goes smoothly.
New prior authorization decision timeframes under CMS-0057-F
The rule establishes specific response windows that payers must meet. These timeframes give you predictable schedules for patient care decisions.
No more open-ended waiting periods. You can mark requests as urgent when clinically appropriate and build care timelines around these decision windows. When a payer misses these deadlines, you have clear documentation of non-compliance.
How AI and automation fit into CMS-0057-F compliance
The rule creates the infrastructure for electronic prior authorization, but your practice still needs tools that meet healthcare compliance standards to use that infrastructure efficiently. Even with digital APIs, someone has to gather clinical information, format requests correctly, and track responses.
AI-powered automation handles these tasks without manual staff intervention. Automation platforms can:
Platforms built by physicians who understand clinical workflows bridge the gap between the rule's requirements and your daily operations. Look for solutions that offer FHIR compliance, seamless EHR integration, broad payer coverage, and transparent reporting on submission outcomes.
How medical practices can prepare for CMS-0057-F
Preparation now prevents rushed implementations later. Focus on three key areas to get ready.
Audit current prior authorization workflows
Map out how prior authorization requests currently move through your practice. Document who submits requests, how long each step takes, what causes denials, and where requests get stuck.
You cannot optimize what you do not measure. Understanding your current state reveals exactly what will change under CMS-0057-F and where you will see the biggest improvements.
Evaluate prior authorization automation technology
Assess solutions that automate request submission, tracking, and response management using your EHR data. The right tool can reduce prior authorization time significantly and improve staff satisfaction.
Key capabilities to look for include EHR integration without manual workarounds, coverage of the payers your practice uses most, accuracy in catching missing information before submission, and clear reporting on trends.
Plan for FHIR API integration with payers
Work with your EHR vendor and payers to establish API connectivity. Ask your vendors specific questions about their timeline, testing environment, support resources, and costs.
Early planning ensures your practice is ready on day one of compliance. Practices that wait until late 2026 will face rushed implementations and confused staff.
Frequently asked questions about CMS-0057-F
Does CMS-0057-F apply to practices that only see Medicare fee-for-service patients?
Traditional Medicare fee-for-service is not covered by this rule, though CMS is separately piloting AI-assisted prior authorization for Part B through the WISeR Model. However, if any of your patients have Medicare Advantage, Medicaid managed care, or exchange plans, those payers must comply.
Will prior authorization requirements disappear under CMS-0057-F?
No. Prior authorization will still exist. The process becomes faster and more transparent through standardized digital workflows, but payers will continue reviewing requests for medical necessity.
What should practices do if their EHR vendor is slow to implement CMS-0057-F?
Start conversations now and ask for their specific roadmap. If they are behind schedule, explore automation platforms that can bridge the gap until your EHR is ready.
Will CMS-0057-F reduce prior authorization denial rates?
The rule makes denial reasons transparent and gives practices tools to understand payer criteria upfront. Practices using automation to catch missing information before submission will see fewer denials.
Get started with CMS-0057-F preparation today
January 2026 arrives faster than you think. Practices that start preparation now will transition smoothly. Those that wait will face rushed implementations and staff confusion.
Audit your current prior authorization workflows and identify the gaps that CMS-0057-F will fill. Understand which payers your practice works with most and prioritize those relationships. A free phone audit can show you how automation streamlines your prior authorization process today and prepares you for CMS-0057-F compliance tomorrow.

Get Started
AI-Enhanced Healthcare with Insight Health


