.png)
Prior authorization is the approval process you must complete before insurance companies agree to cover certain treatments, procedures, or medications. AI prior authorization software automates this traditionally manual process. CMS estimates this costs $34,000 per provider annually.
Your staff spends less time on paperwork and phone calls.
These tools connect directly to your EHR and insurance company portals.
When you order a treatment requiring approval, the software extracts clinical data from the patient's chart. It matches data against payer requirements and submits the request electronically.
The core capabilities include:
- Real-time data extraction: AI pulls clinical information directly from patient records, eliminating manual chart reviews.
- Payer rule matching: The software continuously updates and applies insurance-specific clinical criteria to reduce denials.
- Automated submission: Requests are filled out, signed, and submitted directly to payers without staff intervention.
- Faster decisions: Qualified cases receive authorization decisions in minutes rather than days.
For practices completing dozens of prior authorizations weekly, this automation translates to recovered staff hours and faster patient access to treatment.
How AI prior authorization software works
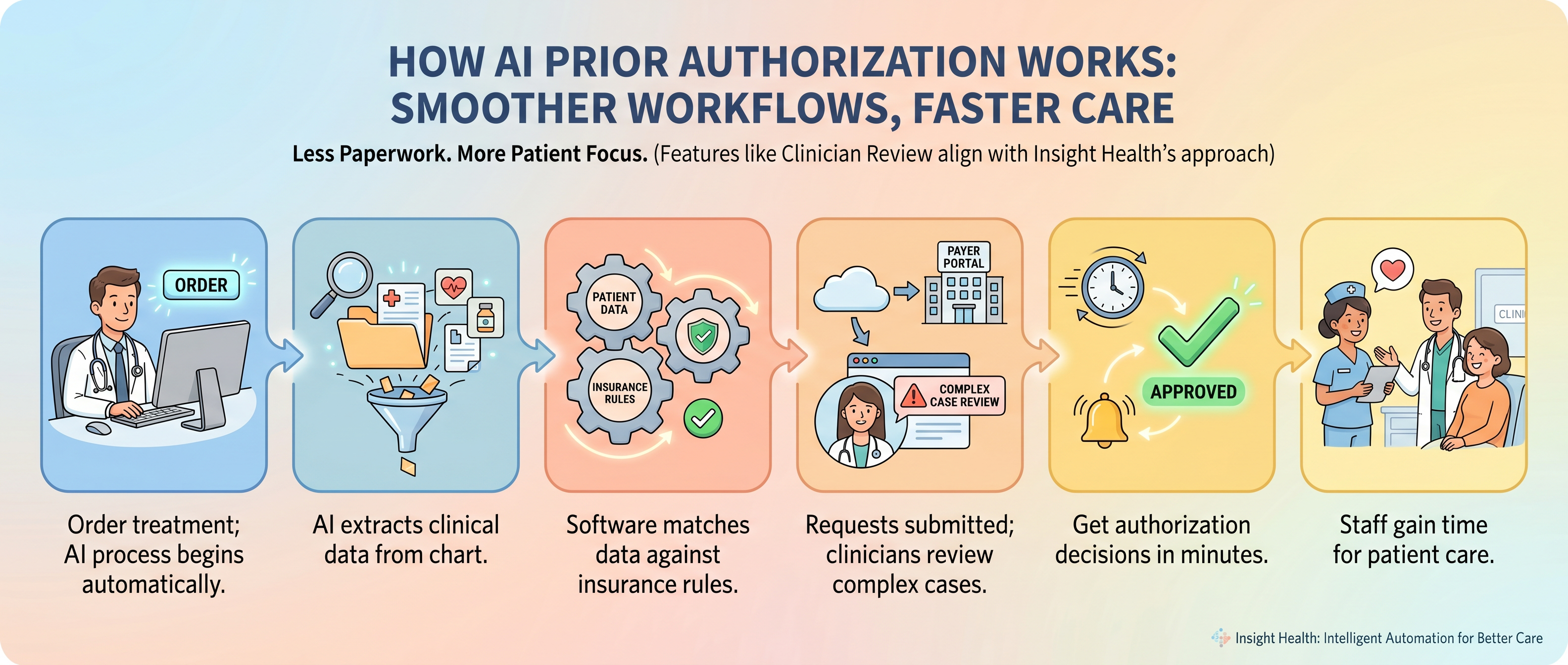
AI prior authorization software operates through a multi-step workflow designed to minimize manual touchpoints while keeping clinicians in control.
When you place an order in your EHR, the AI scans the patient's clinical record and extracts relevant data automatically. This includes diagnosis codes, medications, lab results, and clinical notes. The software identifies whether the treatment or procedure requires prior authorization based on the patient's specific insurance plan.
Next, the software queries its database of insurance policies and clinical criteria. It compares the patient's clinical data against these criteria to determine if the request meets approval requirements.
For complex cases, the AI bundles related clinical information and highlights key evidence supporting medical necessity. Some platforms route these cases to human reviewers who make final determinations.
Once ready, the software submits the request to the payer via direct API connection, electronic submission, or fax. It tracks status in real time and notifies your team of updates or denials. The software also monitors authorization expiration dates and alerts your team to renewals needed before patient appointments.
This end-to-end automation means your staff spends less time chasing paperwork and more time on direct patient care.
7 best AI prior authorization software tools for 2026
The following tools represent the leading AI prior authorization solutions available today. Each serves different practice sizes and specialties, so I have organized them by their primary strengths.
1. Insight Health
Insight Health is the most complete provider-side AI prior authorization solution on this list. It treats PA as a workflow problem beginning at referral, not at order placement. Built by practicing physicians, the platform spans referral intake through documentation, submission, and denial appeals.
Intelligence is active at every stage, not bolted on at the end.
The differentiator is depth of payer intelligence. Insight Health encodes payer-specific clinical criteria at the procedure level. It is tuned for specialties with highest friction: pain management, neurosurgery, orthopedics, gastroenterology, and oncology.
The criteria engine doesn't just check submissions for completeness. It actively shapes documentation upstream, prompting structured capture at the right moment in the visit.
The platform is built modularly. You can deploy the full stack or adopt individual surfaces independently.
Practices can start with the Aura AI Scribe, add referral-moment pre-screening, and layer in submission automation as volume justifies. Insight Health supports today's payer-portal submission paths and is FHIR Da Vinci PAS-ready for the January 2027 CMS-0057-F transition.
The platform is HIPAA and SOC 2 Type II compliant with a standard BAA included. It integrates with Epic, athenahealth, AdvancedMD, DrChrono, eClinicalWorks, and other major EHRs. Outcome-based pricing means you pay only for measurable results such as approved authorizations and reduced denials.
Main features:
- PA eligibility, insurance nuances, and documentation requirements at referral moment.
- External records via pre-visit screening to reduce post-visit denials.
- Specialty-deep payer intelligence per procedure and payer.
- Modular deployment: AI scribe, policy engine, pre-screen, submission, or full workflow.
- Aura AI Scribe with criteria-aware structured capture at point of care.
- Payer portal submissions with FHIR Da Vinci PAS readiness for January 2027.
- Denial parsing and AI appeals tied to specific evidence in notes.
- ICD-10 and CPT coding suggestions to reduce documentation burden.
- HIPAA and SOC 2 Type II compliance with standard BAA.
- Integration with Epic, athenahealth, AdvancedMD, DrChrono, eClinicalWorks, and other major EHRs.
Ideal for: Specialty practices in pain management, neurosurgery, orthopedics, gastroenterology, and oncology where procedure prior authorization is high-volume and high-friction. Practices that want a workflow-integrated solution that activates at referral rather than only at submission. Organizations seeking specialty-deep payer intelligence rather than generic rule libraries.
Pricing: The PA Intelligence Platform uses outcome-based pricing tied to approved authorizations and reduced denials.
2. Availity AuthAI
Availity AuthAI is the AI-powered prior authorization engine from Availity, connecting providers to over 170 insurance plans. The platform delivers authorization recommendations in under 90 seconds by applying each plan's specific medical criteria to your patient's clinical data.
Availity's strength lies in its transparency. Rather than using a black-box machine learning model, AuthAI uses analytical AI grounded in each payer's actual clinical policies.
This means recommendations are fully traceable and auditable, so your team understands exactly why a case was approved or flagged for review. The platform is built for CMS-0057-F compliance with FHIR-native APIs ready for January 2027 requirements.
Ideal for: Practices wanting explainable, transparent AI prior authorization. Organizations concerned about denial bias and auditability.
Pricing: Custom enterprise pricing based on volume and payer network scope.
3. Myndshft
Myndshft is a unified prior authorization solution for both medical and pharmacy benefits. Now part of DrFirst, Myndshft covers approximately 94% of U.S. covered lives through its library of over 600 payer rules.
The platform automates requirement identification, submission, monitoring, and adjudication across multiple submission routes, including payer portals, EDI 278 transactions, and fax. Its self-learning rules engine adapts to policy changes automatically, reducing the manual updates typically required when payers change their clinical criteria.
Ideal for: Mid-sized practices that want AI-driven determination as a centerpiece, not an add-on. Practices managing both medical and pharmacy authorizations.
Pricing: Custom enterprise pricing based on transaction volume and integrations.
4. Banjo Health
Banjo Health provides an AI-assisted prior authorization workflow platform designed primarily for payers and PBMs seeking to streamline their internal review processes. The platform includes BanjoPA for intake-agnostic capture and automated clinical review, plus Composer for building clinical decision trees without code.
Banjo's CARE engine surfaces clinical evidence during review to accelerate decisions while keeping clinicians in control. The platform is HITRUST r2 certified and accepts prior authorization requests from any source, whether fax, digital submission, or portal.
Ideal for: Payers and pharmacy benefit managers. Organizations needing flexible intake from multiple submission sources.
Pricing: Custom pricing based on members, transaction volume, and workflow complexity.
5. Humata Health
Humata Health focuses on eliminating friction in the prior authorization process through intelligent automation embedded directly in your EHR workflow. The platform detects authorization requirements automatically, retrieves payer policies in real time, and bundles clinical evidence for submission.
Humata's PolicyLink feature automatically retrieves and applies payer-specific requirements without manual lookup. The platform includes intelligent gold-carding to reduce repeat authorizations for stable patients. Humata is a designated participant in the CMS WISeR Model for Medicare FFS prior authorization, making it a strong choice for practices serving Medicare populations.
Ideal for: Practices serving Medicare populations. Organizations seeking deep EHR integration and automated policy retrieval.
Pricing: Custom enterprise pricing based on payer connections and integrations.
6. Tandem
Tandem automates the entire prior authorization and medication access journey from prescription to patient delivery. The platform is free for providers and patients, positioning itself as a consumer-friendly alternative to traditional PA software.
Tandem automates prior authorizations, appeal letters, and enrollment forms, then conducts pharmacy and payer calls on behalf of your practice. The platform tracks PA renewals, routes prescriptions to the patient's preferred pharmacy, finds financial assistance programs, and keeps patients updated via text message. Most prior authorizations are completed within 24 hours.
Ideal for: High-prescription clinics, particularly primary care, psychiatry, dermatology, oncology, and rheumatology. Practices wanting a free solution for medication access.
Pricing: Free for providers and patients.
7. Innovaccer
Innovaccer is a data activation platform for health systems seeking to integrate prior authorization into a broader clinical intelligence and population health strategy. The platform unifies multi-source clinical and claims data, then applies AI agents to automate workflows including prior authorization.
Innovaccer's strength is its enterprise-scale data integration and governance. The platform supports FHIR Level 4 interoperability and SMART on FHIR apps, making it flexible for organizations with complex EHR environments.
Ideal for: Large health systems and payers. Organizations with complex data environments needing unified analytics alongside workflow automation.
Pricing: Custom enterprise pricing based on deployment size, users, and scope of modules.
What to look for in AI prior authorization software
When evaluating prior authorization software, prioritize features that reduce manual work while maintaining clinical oversight.
Your software should integrate seamlessly with your specific EHR so prior authorization workflows feel native to your existing processes. Avoid tools requiring staff to toggle between multiple systems. Look for platforms with direct connections to your most common insurance plans, which reduces reliance on fax and phone submissions.
The software should automatically update payer policies and clinical criteria as they change. Manual policy management creates bottlenecks and increases denial rates.
The best tools keep clinicians in control rather than fully automating decisions. Your team should review complex cases and have clear visibility into why the AI recommended approval or denial.
Ensure the platform meets HIPAA and SOC 2 Type II standards. For payer-facing tools, HITRUST certification is increasingly expected. The software should maintain detailed audit trails for compliance and appeal purposes.
Benefits of AI prior authorization software for healthcare practices
Implementing AI prior authorization software delivers measurable benefits across clinical, operational, and financial dimensions.
Patients begin treatment sooner when approvals happen in minutes rather than days. Your nurses, medical assistants, and front-desk team spend less time on authorization calls and paperwork, freeing them to focus on direct patient care.
MGMA reports 92% of practices have hired or reassigned staff solely for prior authorization. This automation reclaims that capacity and reduces burnout.
AI software ensures submissions include all required clinical information and align with payer criteria before submission. This reduces denials and the costly appeal process. Faster authorizations also mean faster treatment delivery and faster claims processing, improving revenue cycle timelines.
Platforms with built-in compliance features and audit trails simplify regulatory reviews and prepare you for CMS requirements like CMS-0057-F. Many platforms also provide analytics on denial patterns, payer trends, and authorization timelines, helping you identify process improvements.
Frequently asked questions about AI prior authorization software
Will AI prior authorization software replace my clinical staff?
No. AI prior authorization software eliminates routine, repetitive tasks so your staff can focus on complex cases and patient care. Your team will still review complex authorizations, handle appeals, and manage exceptions.
How long does implementation typically take for prior authorization software?
Implementation timelines vary based on your EHR system and the software's integration depth. Simple integrations may take weeks while complex enterprise deployments may take months.
Does AI prior authorization software work with regional insurance companies?
Most software supports the largest national payers, but smaller regional insurers may not be included. Verify that your software supports your most common payers before purchasing.
Is patient data safe with AI prior authorization software?
Reputable vendors are HIPAA and SOC 2 Type II compliant with strict data security protocols. Request security documentation and compliance certifications before signing a contract.

Get Started
AI-Enhanced Healthcare with Insight Health


